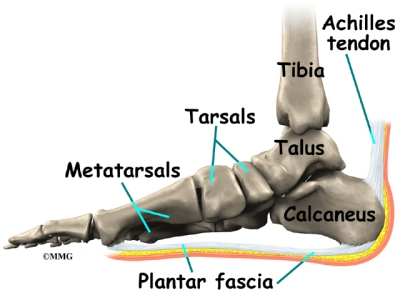
Contracted Toe Medical Operation
 Overview
Overview
A Hammer toe is a term that is commonly used to describe any type of toe deformity. It is a common problem that may or may not be a problem. What does a hammer toe look like? In a hammertoe the deformity usually exists in one toe (at the proximal inter phalangeal joint) - the base of the toe points upward and Hammer toes the end of the toe points down.
Causes
Essentially, hammertoes are caused by an abnormal interworking of the bones, muscles, ligaments and tendons that comprise your feet. When muscles fail to work in a balanced manner, the toe joints can bend to form the hammertoe shape. If they remain in this position for an extended period, the muscles and tendons supporting them tighten and remain in that position. A common factor in development of hammertoe is wearing shoes that squeeze the toes or high heels that jam the toes into the front of the shoe. Most likely due to these factors, hammertoe occurs much more frequently in women than in men.
 Symptoms
Symptoms
The most obvious symptom of hammertoe is the bent, hammer-like or claw-like appearance of one or more of your toes. Typically, the proximal joint of a toe will be bending upward and the distal joint will be bending downward. In some cases, both joints may bend downward, causing the toes to curl under the foot. In the variation of mallet toe, only the distal joint bends downward. Other symptoms may include Pain and stiffness during movement of the toe, Painful corns on the tops of the toe or toes from rubbing against the top of the shoe's toe box, Painful calluses on the bottoms of the toe or toes, Pain on the bottom of the ball of the foot, Redness and swelling at the joints. If you have any of these symptoms, especially the hammer shape, pain or stiffness in a toe or toes, you should consider consulting your physician. Even if you're not significantly bothered by some of these symptoms, the severity of a hammertoe can become worse over time and should be treated as soon as possible. Up to a point hammertoes can be treated without surgery and should be taken care of before they pass that point. After that, surgery may be the only solution.
Diagnosis
Although hammertoes are readily apparent, to arrive at a diagnosis the foot and ankle surgeon will obtain a thorough history of your symptoms and examine your foot. During the physical examination, the doctor may attempt to reproduce your symptoms by manipulating your foot and will study the contractures of the toes. In addition, the foot and ankle surgeon may take x-rays to determine the degree of the deformities and assess any changes that may have occurred.
Non Surgical Treatment
If the problem is caught in the early stages you can avoid hammer toe surgery. One of the easiest methods of treatment is to manipulate the toe out of a bent position then splint and buddy wrap it alongside it?s larger neighbour. This method of hammer toe taping will help the problem to fix itself. Make sure the toe isn?t resuming its bent shape during the recovery. To alleviate some of the painful symptoms of hammer toe avoid wearing high heels or shoes that cramp or stifle your feet. Choosing a pair of minimalist shoes can be an excellent choice for both foot and postural health. Wearing shoes that give the toes plenty of space and are comfortable lined is also a smart choice. Hammer toe recovery starts be treating the toe respectfully. Soft insoles or protection for the corn can also provide additional assistance.
Surgical Treatment
Surgery involves removing a small section of bone from the affected joint through a procedure called arthroplasty. Arthrodesis may also be performed to treat hammertoes, which involves fusing together one of the joints in the toe in order to keep it straight. This procedure requires the use of a metal pin to hold the toe in position while it heals.
 Prevention
Prevention
Certain exercises such as moving and stretching your toe gently with your hands and picking up small or soft objects such as marbles or towels can keep your toe joints flexible, simple exercises can stretch and strengthen your muscles. Limit high-heel use, well-designed flat shoes will be more comfortable than high heels. Don't wear shoes that are too short or too narrow, or too shallow, this is especially important for children going through periods of rapid growth, the toe area should be high enough so that it doesn't rub against the top of your toes.
Over-Pronation
Overview
Overpronation is the most common abnormality found in the foot, and for this reason, is the most studied. The term that most people attribute to overpronation is ?flat feet.? Pronation is the rolling in of the foot and the collapse of the arch. Every person pronates to some extent and this is a necessary moment in the normal walking cycle as it allows the forefoot to make complete contact with the ground. A foot that overpronates acts like a loose bag of bones during the walking cycle. This makes this type of foot very flexible but inefficient. The foot has to work much harder to propel the body, fatiguing easily and placing mechanical stresses on the lower body. We like to use the analogy of digging a hole in the dirt. Overpronating feet are like using a broom to dig the hole. It won?t break down quickly, but you will be digging for a very long time, or until eventually wear and tear will take effect. Wouldn?t you rather have a shovel to work with. This is in essence what an orthotic can do for your feet. This is why orthotics have become an evidence based treatment for so many foot ailments, as they can effectively manage overpronation.Overpronation is when a person pronates too much and for too long. This places excess stress on the tendons and ligaments in the foot and ankle.

Causes
Over-pronation has different causes. Obesity, pregnancy, age or repetitive pounding on a hard surface can weaken the arch leading to over-pronation. Over-pronation is also very common with athletes, especially runners and most of them nowadays use orthotics inside their shoes. Over-pronation affects millions of people and contributes to a range of common complaints including sore, aching feet, ball of foot pain, heel Pain, achilles tendonitis, bunions, shin pain, tired, aching legs, knee pain and lower back pain. The most effective treatment solution for over-pronation is wearing an orthotic shoe insert. Orthotics correct over-pronation, thereby providing natural, lasting pain relief from many common biomechanical complaints.
Symptoms
Symptoms can manifest in many different ways. The associated conditions depend on the individual lifestyle of each patient. Here is a list of some of the conditions associated with over Pronation. Hallux Abducto Valgus (bunions). Hallux Rigidus (stiff 1st toe). Arch Pain. Heel Pain (plantar Facsitus). Metatarsalgia (ball of the foot pain). Ankle Sprains. Shin Splints. Achilles Tendonitis. Osteochondrosis. Knee Pain. Corns & Calluses. Flat Feet. Hammer Toes.
Diagnosis
Look at the wear on your shoes and especially running trainers; if you overpronate it's likely the inside of your shoe will be worn down (or seem crushed if they're soft shoes) from the extra strain.

Non Surgical Treatment
Podiatrists are trained to effectively detect and management over-pronation. You can get a referral to a podiatrist from your GP if you are presenting with the pain typical of over-pronation, or you can seek private podiatric care in anyone of several registered and accredited practices across the country. Your podiatrist will examine your foot and its shape to determine whether or not over-pronation is the cause of your pain. If your podiatrist determines that it is a problem with arch support that is giving you trouble, then they can effectively remedy that lack of support with orthotics.
Prevention
Many of the prevention methods for overpronation-orthotics, for example-can be used interchangeably with treatment methods. If the overpronation is severe, you should seek medical attention from a podiatrist who can cast you for custom-made orthotics. Custom-made orthotics are more expensive, but they last longer and provide support, stability, and balance for the entire foot. You can also talk with a shoe specialist about running shoes that offer extra medial support and firm heel counters. Proper shoes can improve symptoms quickly and prevent them from recurring. Surgery can sometimes help cure and prevent this problem if you suffer from inherited or acquired pes planus deformity. Surgery typically involves stabilizing the bones to improve the foot?s support and function.
How Do I Deal With Severs Disease At Home ?
Overview
What Is Calcaneal Apophysitis? Calcaneal apophysitis is a painful inflammation of the heel?s growth plate. It typically affects children between the ages of 8 and 14 years old, because the heel bone (calcaneus) is not fully developed until at least age 14. Until then, new bone is forming at the growth plate (physis), a weak area located at the back of the heel. When there is too much repetitive stress on the growth plate, inflammation can develop. Calcaneal apophysitis is also called Sever?s disease, although it is not a true ?disease.? It is the most common cause of heel pain in children, and can occur in one or both feet. Heel pain in children differs from the most common type of heel pain experienced by adults. While heel pain in adults usually subsides after a period of walking, pediatric heel pain generally doesn?t improve in this manner. In fact, walking typically makes the pain worse.
Causes
A big tendon called the Achilles tendon joins the calf muscle at the back of the leg to the heel. Sever?s disease is thought to occur because of a mismatch in growth of the calf bones to the calf muscle and Achilles tendon. If the bones grow faster than the muscles, the Achilles tendon that attaches the muscle to the heel gets tight. At the same time, until the cartilage of the calcaneum is ossified (turned into bone), it is a potential weak spot. The tight calf muscle and Achilles tendon cause a traction injury on this weak spot, resulting in inflammation and pain. Sever?s disease most commonly affects boys aged ten to 12 years and girls aged nine to 11 years, when growth spurts are beginning. Sever?s disease heals itself with time, so it is known as self-limiting. There is no evidence to suggest that Sever?s disease causes any long term problems or complications.
Symptoms
Symptoms include complaints of pain or tenderness in the heel (or heels), discomfort when heel is squeezed, limping, and more severe pain after walking, running or playing sports. Sever?s disease is directly related to overuse of the bone and tendons in the heel. This can come from playing sports or anything that involves lots of heel movements and hard shoes such as cleats. It can be associated with starting a new sport, or the start of a new season. It occurs more commonly in children who pronate (feet roll inward), and involves both heels in more than half of patients.
Diagnosis
Sever?s disease can be diagnosed based on your history and symptoms. Clinically, your physiotherapist will perform a "squeeze test" and some other tests to confirm the diagnosis. Some children suffer Sever?s disease even though they do less exercise than other. This indicates that it is not just training volume that is at play. Foot and leg biomechanics are a predisposing factor. The main factors thought to predispose a child to Sever?s disease include decrease ankle dorsiflexion, abnormal hind foot motion eg overpronation or supination, tight calf muscles, excessive weight-bearing activities eg running.
Non Surgical Treatment
Reduce inflammation:
Ice: For at least 20 minutes after activity or when pain increases.
Nonsteroidal anti-inflammatory drugs:(NSAIDs) may also help. Stretch the calf. Increase calf flexibility by doing calf stretches for 30 to 45 seconds several times per day.
Protect the heel: The shoe may need to be modified to provide the proper heel lift or arch support.
Select a shoe with good arch support and heel lift if possible. Try heel lifts or heel cups in sports shoes, especially cleats. Try arch support in cleats if flat feet contribute to the problem.
Take it one step at a time:. Gradually resume running and impact activities as symptoms allow. Sever?s disease usually goes away when the growth plate (apophysis) matures, which should be by age 12 to 13 years in females and 13 to 14 years in males.
Prevention
After the painful symptoms of Sever's disease have gone away, it is important to continue stretching the heel, particularly before a vigorous exercise, and wearing good supportive shoes fitted with children's arch supports. This will prevent heel pain recurrence until the child's heel is fully developed and less prone to injury.
Do I Suffer Adult Aquired FlatFoot ?
Overview
Adult flatfoot may be due to multiple problems including a dysfunctional posterior tibial tendon (PTT), hypermobility and ligamentous laxity, or possibly a coalition that becomes symptomatic. For a vast majority of patients, posterior tibial tendon dysfunction (PTTD) is the cause of symptomatic flatfoot and is the main trigger of surgical reconstruction in flatfoot. The common presenting scenario for adult flatfoot is a case of unilateral flatfoot with pain. Patients will often confirm they always had flat feet but have noticed increased pain and additional collapse in the past few months to years. They may also note increased swelling and a possible concern over one foot increasing in shoe size. After a comprehensive dermatologic, neurologic and vascular assessment, one should direct his or her attention to the musculoskeletal portion of the exam. It is key to examine the foot and leg as a whole in order to determine the proper procedure and consider each phase of the corrective surgery.

Causes
Overuse of the posterior tibial tendon is often the cause of PTTD. In fact, the symptoms usually occur after activities that involve the tendon, such as running, walking, hiking, or climbing stairs.
Symptoms
Symptoms of pain may have developed gradually as result of overuse or they may be traced to one minor injury. Typically, the pain localizes to the inside (medial) aspect of the ankle, under the medial malleolus. However, some patients will also experience pain over the outside (lateral) aspect of the hindfoot because of the displacement of the calcaneus impinging with the lateral malleolus. This usually occurs later in the course of the condition. Patients may walk with a limp or in advanced cases be disabled due to pain. They may also have noticed worsening of their flatfoot deformity.
Diagnosis
There are four stages of adult-acquired flatfoot deformity (AAFD). The severity of the deformity determines your stage. For example, Stage I means there is a flatfoot position but without deformity. Pain and swelling from tendinitis is common in this stage. Stage II there is a change in the foot alignment. This means a deformity is starting to develop. The physician can still move the bones back into place manually (passively). Stage III adult-acquired flatfoot deformity (AAFD) tells us there is a fixed deformity. This means the ankle is stiff or rigid and doesn???t move beyond a neutral (midline) position. Stage IV is characterized by deformity in the foot and the ankle. The deformity may be flexible or fixed. The joints often show signs of degenerative joint disease (arthritis).
Non surgical Treatment
What are the treatment options? In early stages an orthotic that caters for a medially deviated subtalar joint ac-cess. Examples of these are the RX skive, Medafeet MOSI device. Customised de-vices with a Kirby skive or MOSI adaptation will provide greater control than a prefabricated device. If the condition develops further a UCBL orthotic or an AFO (ankle foot orthotic) could be necessary for greater control. Various different forms of surgery are available depending upon the root cause of the issue and severity.

Surgical Treatment
When conservative care fails to control symptoms and/or deformity, then surgery may be needed. The goal of surgical treatment is to obtain good alignment while keeping the foot and ankle as flexible as possible. The most common procedures used with this condition include arthrodesis (fusion), osteotomy (cutting out a wedge-shaped piece of bone), and lateral column lengthening. Lateral column lengthening involves the use of a bone graft at the calcaneocuboid joint. This procedure helps restore the medial longitudinal arch (arch along the inside of the foot). A torn tendon or spring ligament will be repaired or reconstructed. Other surgical options include tendon shortening or lengthening. Or the surgeon may move one or more tendons. This procedure is called a tendon transfer. Tendon transfer uses another tendon to help the posterior tibial tendon function more effectively. A tendon transfer is designed to change the force and angle of pull on the bones of the arch. It's not clear yet from research evidence which surgical procedure works best for this condition. A combination of surgical treatments may be needed. It may depend on your age, type and severity of deformity and symptoms, and your desired level of daily activity.
What Might Cause Achilles Tendonitis ?
Overview
 Tendinitis is the inflammation of a tendon. Tendons are thick cords of tissue that connect muscles to bone. Achilles tendinitis, or an inflammation of the Achilles tendon, is one of the most common causes of foot or ankle pain. Other types of foot/ankle tendinitis include posterior tibial tendinitis and peroneal tendinitis.
Tendinitis is the inflammation of a tendon. Tendons are thick cords of tissue that connect muscles to bone. Achilles tendinitis, or an inflammation of the Achilles tendon, is one of the most common causes of foot or ankle pain. Other types of foot/ankle tendinitis include posterior tibial tendinitis and peroneal tendinitis.
Causes
The calf is under a lot of strain when running: it is not only put on stretch during landing of the foot, but it also has to produce the tension needed to support body weight and absorb the shock of landing. This is what is called an ?eccentric load?. Excessive eccentric loading - either by way of a dramatic increase in mileage, or excessive hill running, or faulty running posture - could very well be the cause of a runner?s achilles tendinitis. The calf strain translates downward into the achilles tendon where it attaches to the heel, and inflammation ensues. Inflammation then causes scarring and fibrosis of tissues, which in turn inflicts pain upon stretching or use. Risk factors for Achilles tendinitis also include spending prolonged amounts of time standing or walking.
Symptoms
If you have Achilles tendinitis or Achilles enthesopathy, you are likely to experience the following symptoms. Pain. You may notice aching, burning, or tearing pains at the back of your heel or above the ankle. The pain can range from mild to very severe and disabling. It is most noticeable in the following circumstances. After resting. Many people report that pain increases when they first get out of bed in the morning or after sitting for a period of time. After exercise. Pain may increase if you exercise or stand for a period of time. A lump. In some cases, a tender lump can develop at the site of the injured tendon (tendinosis). Bone spurs. When the injury occurs at the point where the tendon attaches to the foot, a bone spur may develop on the heel.
Diagnosis
In diagnosing Achilles tendonitis or tendonosis, the surgeon will examine the patient?s foot and ankle and evaluate the range of motion and condition of the tendon. The extent of the condition can be further assessed with x-rays or other imaging modalities.
Nonsurgical Treatment
The aim, when treating Achilles tendinitis, is to relieve pain and reduce swelling. The kind of treatment used can vary, based on the severity of the condition and whether or not the patient is a professional athlete. After diagnosis, the doctor will decide which method of treatment is required for the patient to undergo, it is likely that they will suggest a combination. Stretching achilles tendon, a doctor might show the patient some stretching exercises that help the Achilles tendon heal, as well as preventing future injury. Methods used to treat Achilles tendinitis include, ice packs - applying these to the tendon, when in pain or after exercising, can alleviate the pain and inflammation. Resting, this gives the tissue time to heal. The type of rest needed depends on the severity of the symptoms. In mild cases of Achilles tendinitis, it may mean just reducing the intensity of a workout, in severe cases it might mean complete rest for days or weeks. Elevating the foot, swelling can be reduced if the foot is kept raised above the level of the heart. Exercise and stretching, a doctor might show the patient some stretching exercises that help the Achilles tendon heal, as well as preventing future injury. They may, instead, refer the patient to a physiotherapist or another specialist. The exercises learned will improve the flexibility of the area and likely increase calf strength. Pain relievers - non-steroidal anti-inflammatory drugs (NSAIDS), such as ibuprofen can reduce pain and swelling. If you suffer from asthma, kidney disease or liver disease do not take NSAIDs without first checking with your doctor. Steroid injections, these can reduce tendon swelling, but should be performed with caution, as this process has been associated with a greater risk of tendon rupture. A doctor would likely perform the injection while scanning the area with ultrasound to reduce this risk. Compression bandages and orthotic devices, such as ankle supports and shoe inserts can aid recovery as they take the stress off the Achilles tendon.

Surgical Treatment
Treating this surgically, there are numerous methods to repair the tendon. Most commonly, Achilles tendon is exposed through an incision at the back of the ankle. After identifying both ends of ruptured tendon, the edges got trimmed and then both ends were sutured together with optimal tension. To get a better outcome with fixation, an anchor may have to be in place in calcaneus, provided the rupture is very low. Care must be taken to avoid injuries to the nerves located adjacent to the tendon.
Prevention
Suggestions to reduce your risk of Achilles tendonitis include, icorporate stretching into your warm-up and cool-down routines. Maintaining an adequate level of fitness for your sport. Avoid dramatic increases in sports training. If you experience pain in your Achilles tendon, rest the area. Trying to ?work through? the pain will only make your injury worse. Wear good quality supportive shoes appropriate to your sport. If there is foot deformity or flattening, obtain orthoses. Avoid wearing high heels on a regular basis. Maintaining your foot in a ?tiptoe? position shortens your calf muscles and reduces the flexibility of your Achilles tendon. An inflexible Achilles tendon is more susceptible to injury. Maintain a normal healthy weight.
What Will Cause Pain On The Heel And How To Remedy It

Overview
Heel pain is the most common musculoskeletal complaint of patients presenting to podiatric practitioners throughout the country. It is well-recognized that subcalcaneal pain syndrome, commonly attributed to plantar fascitis, is a disease entity that is increasing in its incidence, owing partly to the fact that it has a predilection for people between the age of 40 and 60, the largest age segment in our population.
Causes
Plantar fasciitis occurs when the ligament in your foot arch is strained repeatedly, which causes tiny tears and significant pain. There are several possible causes for this condition. Excessive pronation, or overpronation, which happens when your feet roll excessively inward as you walk. Flat feet or high arches. Walking, standing, or running for long periods of time, particularly on hard surfaces (a common problem for athletes). Excess weight, such as overweight or obesity. Shoes that are worn out or don’t fit well. Tight calf muscles or Achilles tendons.
Symptoms
Plantar fasciitis is usually found in one foot. While bilateral plantar fasciitis is not unheard of, this condition is more the result of a systemic arthritic condition that is extremely rare in an athletic population. There is a greater incidence of plantar fasciitis in males than females (Ambrosius 1992). While no direct cause could be found it could be argued that males are generally heavier which, when combined with the greater speeds, increased ground contact forces, and less flexibility, may explain the greater injury predisposition. The most notable characteristic of plantar fasciitis is pain upon rising, particularly the first step out of bed. This morning pain can be located with pinpoint accuracy at the bony landmark on the anterior medial tubercle of the calcaneus. The pain may be severe enough to prevent the athlete from walking barefooted in a normal heel-toe gait. Other less common presentations include referred pain to the subtalar joint, the forefoot, the arch of the foot or the achilles tendon (Brantingham 1992). After several minutes of walking the pain usually subsides only to re turn with the vigorous activity of the day's training session. The problem should be obvious to the coach as the athlete will exhibit altered gait and/ or an abnormal stride pattern, and may complain of foot pain during running/jumping activities. Consistent with plantar fascia problems the athlete will have a shortened gastroc complex. This can be evidenced by poor dorsiflexion (lifting the forefoot off the ground) or inability to perform the "flying frog" position. In the flying frog the athlete goes into a full squat position and maintains balance and full ground contact with the sole of the foot. Elevation of the heel signifies a tight gastroc complex. This test can be done with the training shoes on.
Diagnosis
Your doctor will check your feet and watch you stand and walk. He or she will also ask questions about your past health, including what illnesses or injuries you have had. Your symptoms, such as where the pain is and what time of day your foot hurts most. How active you are and what types of physical activity you do. Your doctor may take an X-ray of your foot if he or she suspects a problem with the bones of your foot, such as a stress fracture.
Non Surgical Treatment
To alleviate the stress and pain on the fascia, the person can take shorter steps and avoid walking barefoot. Activities that involve foot impact, such as jogging, should be avoided. The most effective treatments include the use of in-shoe heel and arch cushioning with calf-stretching exercises and night splints that stretch the calf and plantar fascia while the patient sleeps. Prefabricated or custom-made foot orthotics may also alleviate fascial tension and symptoms. Other treatments may include activity modifications, NSAIDs, weight loss in obese patients, cold and ice massage therapy, and occasional corticosteroid injections. However, because corticosteroid injections can predispose to plantar fasciosis, many clinicians limit these injections. For recalcitrant cases, physical therapy, oral corticosteroids, and cast immobilization should be used before surgical intervention is considered. A newer form of treatment for recalcitrant types of plantar fasciosis is extracorporeal pulse activation therapy (EPAT), in which low-frequency pulse waves are delivered locally using a handheld applicator. The pulsed pressure wave is a safe, noninvasive technique that stimulates metabolism and enhances blood circulation, which helps regenerate damaged tissue and accelerate healing. EPAT is being used at major medical centers.

Surgical Treatment
Plantar fasciotomy is often considered after conservative treatment has failed to resolve the issue after six months and is viewed as a last resort. Minimally invasive and endoscopic approaches to plantar fasciotomy exist but require a specialist who is familiar with certain equipment. Heel spur removal during plantar fasciotomy has not been found to improve the surgical outcome. Plantar heel pain may occur for multiple reasons and release of the lateral plantar nerve branch may be performed alongside the plantar fasciotomy in select cases. Possible complications of plantar fasciotomy include nerve injury, instability of the medial longitudinal arch of the foot, fracture of the calcaneus, prolonged recovery time, infection, rupture of the plantar fascia, and failure to improve the pain. Coblation (TOPAZ) surgery has recently been proposed as alternative surgical approaches for the treatment of recalcitrant plantar fasciitis.
Prevention
Every time your foot strikes the ground, the plantar fascia is stretched. You can reduce the strain and stress on the plantar fascia by following these simple instructions: Avoid running on hard or uneven ground, lose any excess weight, and wear shoes and orthotics that support your arch to prevent over-stretching of the plantar fascia.
What Is Painful Heel And The Way To Treat It

Overview
Plantar Fasciitis is actually, in most cases, plantar fasciosis but it’s a bit like pen/biro or hoover/vacuum. The term ‘-itis‘ means ‘inflammation’. This is a term we use for this problem in the early stages of damage because it usually is quite literally an inflammation of part of the plantar fascia. So, what is commonly known as ‘plantar fasciitis’ is really ‘plantar fasciosis’ - a degradation or degeneration of the collagen fibres because of prolonged (most of your adult life) unsustainable stress being applied to the fascia. So, we call it plantar fasciitis but it usually hasn’t been an ‘-itis‘ for years and that is why in many cases anti-inflammatory drugs do not help ease the pain of walking. This is also why most sufferers experience pain first thing in the morning. If inflammation was the source of discomfort then why would it hurt after a nights rest and the good old drugs pumping through your system.
Causes
It usually starts following an increase in activity levels. Increase in weight. Standing for long periods. Poor footwear. Tight muscle groups. Abnormal pressure on the plantar Fascia can be caused by any of the above. The plantar fascia becomes inflamed and tiny rips can occur where it attaches into the inside of the heel bone. The area becomes inflamed and swollen, and it is the increase in fluid to the area that accumulates when weight is taken off the area that then causes the pain on standing.
Symptoms
Plantar fasciitis typically causes a stabbing pain in the bottom of your foot near the heel. The pain is usually worst with the first few steps after awakening, although it can also be triggered by long periods of standing or getting up from a seated position.
Diagnosis
To arrive at a diagnosis, the foot and ankle surgeon will obtain your medical history and examine your foot. Throughout this process the surgeon rules out all the possible causes for your heel pain other than plantar fasciitis. In addition, diagnostic imaging studies such as x-rays or other imaging modalities may be used to distinguish the different types of heel pain. Sometimes heel spurs are found in patients with plantar fasciitis, but these are rarely a source of pain. When they are present, the condition may be diagnosed as plantar fasciitis/heel spur syndrome.
Non Surgical Treatment
Many cases of plantar fasciitis can be treated with simple, conservative measures. These include ice packs, stretching exercises, anti-inflammatory medications, orthotic devices (custom molded orthotics), and physical therapy. It’s important to consult your doctor before you take any medications to treat this condition. In chronic or persistent cases, one of three techniques may be used to treat plantar fasciitis. Extracorporeal Shock Wave Treatment (ESWT). TOPAZ treatment. Platelet Rich P
lasma therapy.
Surgical Treatment
When more-conservative measures aren't working, your doctor might recommend steroid shots. Injecting a type of steroid medication into the tender area can provide temporary pain relief. Multiple injections aren't recommended because they can weaken your plantar fascia and possibly cause it to rupture, as well as shrink the fat pad covering your heel bone. Extracorporeal shock wave therapy. In this procedure, sound waves are directed at the area of heel pain to stimulate healing. It's usually used for chronic plantar fasciitis that hasn't responded to more-conservative treatments. This procedure may cause bruises, swelling, pain, numbness or tingling and has not been shown to be consistently effective. Surgery. Few people need surgery to detach the plantar fascia from the heel bone. It's generally an option only when the pain is severe and all else fails. Side effects include a weakening of the arch in your foot.
What Is Plantar Fasciitis And How You Can Overcome It

Overview
Plantar fasciitis often occurs in middle-age. It also occurs in people who spend long hours standing on their feet at work, like athletes or soldiers. It can happen in one foot or both feet. It is common in sports like long distance running, dancing etc. Athletes who overpronate (rolling in or flattening feet) are especially at risk as the biomechanics of their feet place more stress to the band. Plantar fasciitis can take a long time to heal. Six months is the average time reported in medical research. There are some who will get cured after a few weeks and for others it will take more than a year. It can also become a chronic condition in which case some sort of treatment will always be needed to prevent the pain from coming back. As sooner as the condition is treated chances are it will not get chronic or in other words if you treat plantar fasciitis sooner you will get cured faster.
Causes
Because the plantar fascia supports your foot and gets used every time you take a step, it has to absorb a large amount of stress and weight. If too much pressure is put on the plantar fascia, the fibers can become damaged or start to tear. The body responds by causing inflammation in the affected area. This is what causes the pain and stiffness of plantar fasciitis. Things that can increase the risk of plantar fasciitis include tight calf muscles. Tight calves make it harder to flex your foot, and this puts more stress on the plantar fascia. Weight. Carrying a few extra pounds puts added pressure on your feet every time you take a step. Activities that put a lot of stress on the feet. This includes things like running, hiking, dancing, and aerobics. Bad shoes. Footwear that doesn't give your foot the support it needs increases your risk of plantar fasciitis. You'll want to ditch any shoes that have thin soles or inadequate arch support, or ones that don't fit your feet properly. Routinely wearing high heels can also cause your Achilles tendon to contract over time, making it harder to flex your foot. Jobs that involve a lot of standing or walking on hard surfaces. Jobs that keep you on your feet all day, like waiting tables or working in a store, can cause damage to your plantar fascia. High arches, flat feet, or other foot problems. The shape of your foot can affect the way your weight is distributed on your feet when you stand. If weight distribution is a bit off, it can add to a person's risk of plantar fasciitis. How someone walks can increase the stress on certain parts of the foot too.
Symptoms
The symptoms of plantar fasciitis include pain in the bottom of your foot, especially at the front or centre of the heel bone, pain that is worse when first rising in the morning (called "first-step pain"), when first standing up after any long period of sitting, or after increased levels of activity especially in non-supportive shoes. Seek medical advice about plantar fasciitis if you have heel pain or pain in the bottom of your foot, especially when you get up in the morning, that does not respond to treatment or if there is redness or bruising in the heel.
Diagnosis
Plantar fasciosis is confirmed if firm thumb pressure applied to the calcaneus when the foot is dorsiflexed elicits pain. Fascial pain along the plantar medial border of the fascia may also be present. If findings are equivocal, demonstration of a heel spur on x-ray may support the diagnosis; however, absence does not rule out the diagnosis, and visible spurs are not generally the cause of symptoms. Also, infrequently, calcaneal spurs appear ill defined on x-ray, exhibiting fluffy new bone formation, suggesting spondyloarthropathy (eg, ankylosing spondylitis, reactive arthritis. If an acute fascial tear is suspected, MRI is done.
Non Surgical Treatment
Many cases of plantar fasciitis can be treated with simple, conservative measures. These include ice packs, stretching exercises, anti-inflammatory medications, orthotic devices (custom molded orthotics), and physical therapy. It’s important to consult your doctor before you take any medications to treat this condition. In chronic or persistent cases, one of three techniques may be used to treat plantar fasciitis. Extracorporeal Shock Wave Treatment (ESWT). TOPAZ treatment. Platelet Rich P
lasma therapy.

Surgical Treatment
Most practitioners agree that treatment for plantar fasciitis is a slow process. Most cases resolve within a year. If these more conservative measures don't provide relief after this time, your doctor may suggest other treatment. In such cases, or if your heel pain is truly debilitating and interfering with normal activity, your doctor may discuss surgical options with you. The most common surgery for plantar fasciitis is called a plantar fascia release and involves releasing a portion of the plantar fascia from the heel bone. A plantar fascia release can be performed through a regular incision or as endoscopic surgery, where a tiny incision allows a miniature scope to be inserted and surgery to be performed. About one in 20 patients with plantar fasciitis will need surgery. As with any surgery, there is still some chance that you will continue to have pain afterwards.
Prevention
Maintain a healthy weight. This minimizes the stress on your plantar fascia. Choose supportive shoes. Avoid high heels. Buy shoes with a low to moderate heel, good arch support and shock absorbency. Don't go barefoot, especially on hard surfaces. Don't wear worn-out athletic shoes. Replace your old athletic shoes before they stop supporting and cushioning your feet. If you're a runner, buy new shoes after about 500 miles of use. Change your sport. Try a low-impact sport, such as swimming or bicycling, instead of walking or jogging. Apply ice. Hold a cloth-covered ice pack over the area of pain for 15 to 20 minutes three or four times a day or after activity. Or try ice massage. Freeze a water-filled paper cup and roll it over the site of discomfort for about five to seven minutes. Regular ice massage can help reduce pain and inflammation. Stretch your arches. Simple home exercises can stretch your plantar fascia, Achilles tendon and calf muscles.
Symptoms Of Joint Pain in the Foot
Metatarsal pain, often referred to as metatarsalgia, can be caused by several foot conditions, including Freiberg's disease, Morton's neuroma and sesamoiditis. According to a 2003 article in the British Journal of Sports Mallet Toe Medicine,” a flat or high arch is one of many risk factors for lower extremity injuries including foot injuries. Poor circulation occurs when there is not enough blood supplied to an area to meet the needs of the cells.
These conditions include different types of arthritis , osteonecrosis , neuromas , tumors, or infections. Lastly, traumatic injuries, including fractures and ligament tears, can cause this type of foot pain. Treatment of foot pain often consists of anti-inflammatory medications , footwear modifications, and inserts for your shoes. When buying footwear, look for shoes with a wide toebox, good support, and avoid high heels. These pads help to take pressure off the ball of the foot. If some simple steps do not alleviate your symptoms, you should see your doctor to ensure you are receiving adequate treatment. In some rare situations, patients don't find relief with shoe modifications, and may require a surgical procedure. Remember that our shoes protect us from injury.
If you see just a thin line connecting the ball of your foot to your heel, you have high arches. If you have flat feet or high arches, you're more likely to get plantar fasciitis, an inflammation of the tissue along the bottom of your foot. Without proper arch support, you can have pain in your heels, arch, and leg. You can also develop bunions and hammertoes, which can become painful,” says Marlene Reid, a podiatrist, or foot and ankle doctor, in Naperville, IL. Shoes with good arch support and a slightly raised heel can help ward off trouble. Laces, buckles, or straps are best for high arches. See a foot doctor to get fitted with custom inserts for your shoes. Good running shoes, for example, can prevent heel pain, stress fractures , and other foot problems that can be brought on by running. A 2-inch heel is less damaging than a 4-inch heel. If you have flat feet, opt for chunky heels instead of skinny ones, Reid says.

Rheumatoid arthritis causes forefoot deformity and often may cause displacement and even dislocation of the metatarsal joints themselves. Morton's Neuroma can also be a source of metarsalgia and is characterized by pain in the forefoot. Sesamoiditis is located on the plantar surface of the foot and will be located near the first metatarsal phalangeal joint.

Junctional Epidermolysis Bullosa: A condition that causes blistering of the skin because of a mutation of a gene which in normal conditions helps in the formation of thread-like fibers that are anchoring filaments, which fix the epidermis to the basement membrane. Kanner Syndrome: Also referred to as Autism, this is one of the neuropsychiatric conditions typified by deficiencies in communication and social interaction, and abnormally repetitive behavior. Kaposi's Sarcoma: A kind of malignancy of the skin that usually afflicts the elderly, or those who have problems in their immune system, like AIDS. For example, a year of perfect health is regarded as equivalent to 1.0 QALY.
Print "Symptoms Associated With Side Of Foot Pain"
One of the hardest things to detect is the foot pain bone that is causing a severe foot pain on top of the foot of many women. Our feet are the most used (and abused) part of our body. Are you one of those people who are said to be flat footed? As humans are bipeds, they depend on their feet all day long. Foot pain should not be a part of your daily life.
There is a nerve that runs close to this area and may contribute to the pain which occurs. Haglunds deformity is a bony growth on the back of the heel bone. It irritates the bursa and the skin behind the heel bone. It is commonly called a "pump bump." It develops when the back of your shoe repeatedly rubs against the back of the heel. This irritates the bursa and skin that is above the bone. It is caused by overuse during strenuous exercise, particularly running and high-impact aerobics. Overall, normally occurring flat feet in adults do not cause many functional problems. EBSCO Information Services is fully accredited by URAC URAC is an independent, nonprofit health care accrediting organization dedicated to promoting health care quality through accreditation, certification and commendation. Walking barefoot is often too painful.
The 61-year-old man called police at about 3 a.m. saying that he thought he was missing three toes and part of his right foot. Often people with diabetes lose their toes, so it is curious as to whether or not the dog knew that the man had a condition in which he'd lose his toes anyway at some point. According to the University of Maryland Medical Center, about 75 percent of Americans will experience foot pain at some point in their lives ( UMMC , 2009). The pain can range from mild to severe, and it may last a short time or be an ongoing issue.
Blood glucose levels under control: Meal planning, regular blood glucose monitoring, substantial activity and right diabetes medications including insulin can all go a long way toward relieving the pain associated with the nerve damage. Look them over: Provide your feet a careful going-over every night to make sure that you haven't developed a cut, scrape, sore, blister or any other tiny problem.
One of the most common causes is improper walking habits, i.e., exerting weight or pressure on the metatarsals while walking or running which can lead to pain at night. Symptoms include sharp pain in the middle part of the foot, callousing around the toes, and tingling sensation and severe pain while walking or standing. Pain in the middle of the leg, i.e. in the metatarsals is also one of the symptoms of arthritis.

Participants were asked to indicate when the sensation of pressure changed to onset of pain. The paper grip test was used as a clinical measure of hallux plantarflexion strength 38 , 39 Participants completed three trials of three seconds, and a pass was recorded if the individual could hold the paper under the hallux against resistance for all trials.

Light and washable, they also have specially designed air vents to help keep your feet cool. We'll also include this bottle of soothing peppermint lotion to invigorate your feet and your spirit... And our special sandal adapters, so you'll never be without your Walkfits. It inhibits and kills fungus and bacteria, so no more stinky, sticky feet. And don't forget, we have holes in the Walkfit to keep your feet cool all the time.

Health 4 Clues Ease Your Milia Treatments Coding
Last night I was sat grating the hard skin off my feet (as you do!) and my bf was mocking me, and totally grossed out by it. Make sure you pamper your feet properly and provide a good care in order to get smooth and healthy feet. Dry, cracked feet are unsightly and painful.
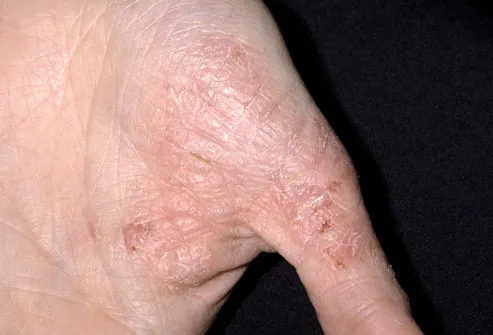
However if you use the right medication, athletes foot can be eliminated through the body system. The reaction occurs based on the body's immune system; however it's always better to exercise proper foot care if you do contract the fungus. This isn't true as shoes with good ventilation don't create moist and warm conditions or lead to athlete's foot. Take preventive care by wearing cotton socks, washing socks everyday and drying the feet after washing or bathing. Now that all these myths have been clarified, just follow a strict and regular hygiene regimen to prevent athlete's foot. Self treatment may lead to more significant problem.
Long hours of work under conditions of stress put an extra burden on the feet. When your feet get painful you concentrate on them instead of the work. When feet become strained and painful they should be studied by an orthopedic surgeon. Don't ignore pain: Painful feet are not normal.

Hands at times also get infected with calluses, but the use of pumice stone is not advised for removal of calluses on hands. The process is a bit slow, but the treatment is permanent and guaranteed without any side effect. There are surgical treatments as well where your doctor will cut the hard skin but only few people resort to this option. As far as medication is concerned salicylic acid ointments is often used to remove the hard portions of the skin. Complications caused by calluses should be consulted with podiatrist as it can also cause infection in certain number of ways. The treatment of callus depends upon its nature and severity. But some of the treatments out there are very hard and damaging to your skin.
Alcohol abuse, thyroid dysfunction, thrombocytopenia (abnormally low platelets that help blood clot) and gastric restriction in obesity can also produce symptoms of burning feet. A pinched nerve where the nerve enters the foot from the ankle, or between the 3rd and 4th toes can also cause burning feet. Corns and callusesare the most common foot problems caused by a person's shoes and the amount of walking they do. Corns are a thickening of the outer layer of the skin, usually on the upper aspect of the toes and often caused by ill-fitting or tight shoes. In some cases the tip of toes have corns.